Executive Summary
Neck pain is often dismissed as a minor musculoskeletal issue, but when it appears alongside high blood pressure (hypertension), it can signal a critical health emergency requiring immediate medical attention.
This guide explains the complex link between neck pain and hypertension, distinguishing between common causes and dangerous “red flag” scenarios like malignant hypertension—a life-threatening condition.
You will learn to recognise key symptoms, understand how blood pressure medications can affect your neck, and discover practical steps for safe monitoring and when to seek urgent care from the NHS. We incorporate the latest medical perspectives, including insights on structural causes like cervical instability, to provide a comprehensive, authoritative resource for your health.
The Critical Link Between Your Neck and Blood Pressure
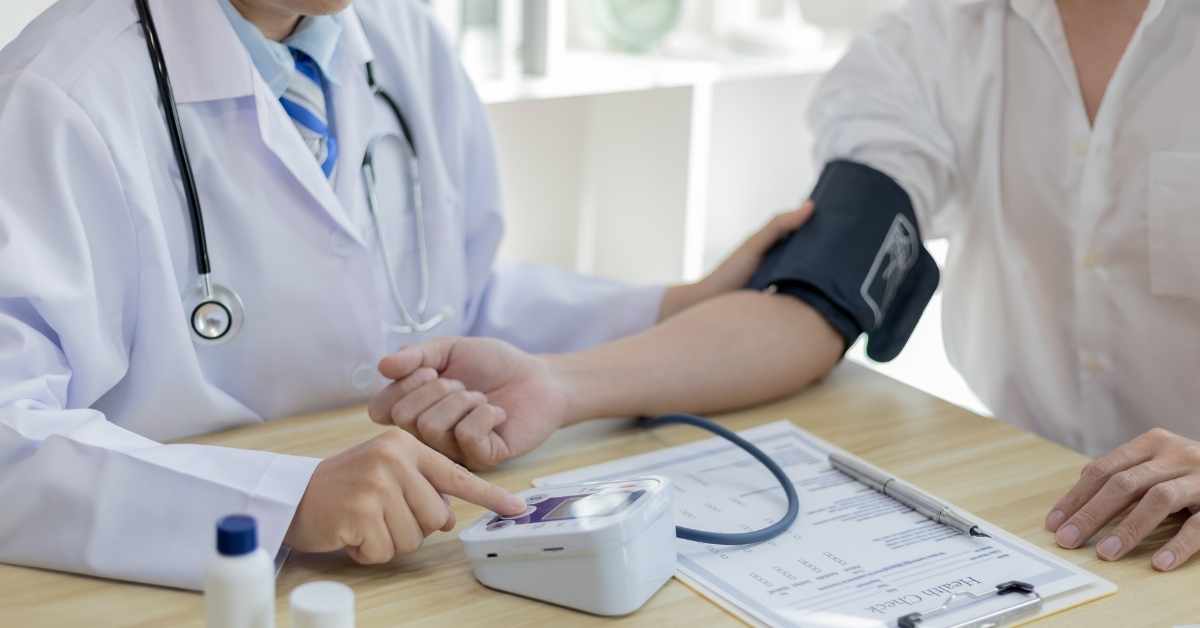
The connection between neck discomfort and high blood pressure is more than coincidental; it’s often physiological. While many cases of neck pain are benign, its occurrence with hypertension warrants careful attention.
For most individuals, hypertension develops silently over years due to lifestyle factors or genetics. However, sudden or severe neck pain, especially at the base of the skull, can indicate a dangerous spike in blood pressure that is putting immense strain on your body’s systems.
Fundamentally, your body regulates blood pressure through a sophisticated network involving the heart, blood vessels, brain, and key nerves. Two nerves are particularly crucial: the vagus nerve and the glossopharyngeal nerve.
These nerves run through the upper cervical spine (your neck) and act as communication cables, sending signals from pressure sensors in your arteries to your brainstem, which then instructs your heart to beat slower or faster to maintain stable pressure.
Research indicates that instability or misalignment in the upper cervical vertebrae can potentially impinge or disrupt these nerves, leading to dysregulated blood pressure. This can manifest as unpredictable highs and lows that don’t respond typically to standard medications.
Understanding this link is the first step in differentiating a routine tension headache from a symptom that demands a call to 111 or a trip to A&E.
Recognising the Symptoms: From Common to Critical

Neck pain associated with high blood pressure often has distinct characteristics that set it apart from everyday stiffness or strain.
Typical Presentation of a Hypertensive Headache & Neck Pain
-
Location and Quality: The pain is often described as a pressing or tightening sensation that starts at the back of the head (occipital region) and can radiate into the neck and shoulders. It’s frequently bilateral, affecting both sides.
-
Timing: These headaches and neck aches are notorious for being worse first thing in the morning, as blood pressure naturally rises upon waking.
-
Accompanying Symptoms: They may occur alongside other signs of elevated blood pressure, such as dizziness, visual disturbances (like blurred vision), facial flushing, or a feeling of fullness in the head.
“Red Flag” Symptoms: When Neck Pain Signals an Emergency
Certain symptoms transform neck pain from a concern into a medical emergency. This combination may indicate malignant hypertension or hypertensive encephalopathy—conditions where extremely high blood pressure is causing acute damage to organs, including the brain.
-
Sudden, Severe Pain: An explosive or “thunderclap” headache with intense neck stiffness.
-
Neurological Changes: Confusion, drowsiness, vision loss, seizures, or weakness on one side of the body.
-
Other Critical Signs: Chest pain, severe shortness of breath, or nausea and vomiting.
If you experience high blood pressure with neck pain alongside any of these red flags, seek emergency medical attention immediately by calling 999.
Can Hypertension or Its Treatment Cause Neck Pain?
The relationship is multifaceted, involving both the condition itself and, in some cases, the medications used to treat it.
1. Hypertension as a Direct Cause
Chronically high blood pressure increases the force against all your arterial walls. In the neck, this can strain muscles and connective tissue. More critically, a hypertensive crisis (a severe, rapid increase in pressure) can cause a dangerous rise in intracranial pressure.
A seminal 1997 case study in the Emergency Medicine Journal highlighted that severe, unexplained neck pain can be a presenting symptom of malignant hypertension, possibly due to incipient tonsillar herniation—where brain tissue is pushed downward due to extreme pressure. This is a rare but life-threatening mechanism.
2. Blood Pressure Medications as an Indirect Cause
Some medications used to treat high blood pressure list muscle pain or cramping as a potential side effect. While not common, certain calcium channel blockers or statins (often prescribed for related cholesterol issues) can contribute to generalised muscle aches, which may be felt in the neck and shoulders.
It is crucial never to stop taking prescribed medication due to side effects without first consulting your GP, who can adjust your treatment plan safely.
3. The Structural Hypothesis: Cervical Instability
An emerging perspective discussed in specialist literature suggests a structural link. The theory posits that ligament laxity or instability in the upper cervical spine (the C1-C2 vertebrae) can physically irritate or compress the vagus and glossopharyngeal nerves.
This interference may disrupt the baroreceptor reflex—the body’s primary system for maintaining stable blood pressure—potentially leading to secondary hypertension that is difficult to control with standard therapies.
This area requires more research but is considered for patients with concurrent neck instability, trauma history, and treatment-resistant hypertension.
Diagnostic Pathways: What to Expect from Your GP
If you present with neck pain and high blood pressure, your GP will follow a systematic approach to rule out serious causes and identify the underlying issue.
-
Detailed History: They will ask about the pain’s onset, character, duration, and any associated symptoms. Be prepared to discuss your full medical history and all medications.
-
Accurate Blood Pressure Measurement: This is essential. Your GP may recommend ambulatory blood pressure monitoring (ABPM), where you wear a device for 24 hours, to get a true average and identify patterns. Using a reliable home blood pressure monitor is also key for long-term management. For guidance on selecting one, see our guide: How to Choose the Best Home Blood Pressure Monitor in the UK.
-
Physical Examination: This includes a neurological exam to check reflexes, strength, and sensation, and a careful examination of your neck.
-
Investigations: Based on the initial assessment, tests may include:
-
Blood Tests: To check kidney function, electrolytes, and hormone levels.
-
Imaging: An MRI or CT scan of the brain and cervical spine may be ordered if there is suspicion of malignant hypertension, neurological deficit, or structural cervical issues.
-
Echocardiogram: To assess if high blood pressure has affected the heart’s structure.
-
Practical Management and Relief Strategies

Management focuses on two parallel tracks: controlling blood pressure and safely alleviating neck discomfort.
For Blood Pressure Control
-
Lifestyle Modifications: These are the cornerstone. Adopt a low-sodium diet, engage in regular moderate exercise, maintain a healthy weight, limit alcohol, and practice stress-reduction techniques like mindfulness.
-
Medication Adherence: Take all prescribed medications consistently. If side effects are problematic, your GP can adjust the type or dosage.
-
Regular Monitoring: Use a validated home monitor to track your readings. Tools like the Blood Pressure Average Calculator can help you understand your true baseline by averaging multiple readings, providing more useful data for your doctor than a single measurement.
For Neck Pain Relief (When Not an Emergency)
-
Heat Therapy: A warm compress or heating pad on the neck for 15-20 minutes can relax tense muscles.
-
Gentle Stretching: Slow, controlled neck stretches (avoiding rapid circles) can improve mobility. A physiotherapist can provide a safe routine.
-
Posture Correction: Ensure your workstation is ergonomically set up to avoid forward head posture, which strains cervical muscles.
-
Sleep Position: Sleeping on your back or side with a supportive pillow that keeps your neck aligned with your spine can reduce strain. The best sleeping position for blood pressure is generally on your left side, which can also aid circulation.
-
Over-the-Counter Pain Relief: Short-term use of paracetamol may be suitable, but always check with a pharmacist or GP, especially if you are on other medications.
Frequently Asked Questions (FAQs)
Does hypertension cause neck pain?
Yes, it can. Chronically high blood pressure can contribute to muscular tension and headaches that radiate to the neck. In acute, severe cases (a hypertensive crisis), the dramatic increase in pressure can cause sudden, severe neck pain and headache, which is a medical emergency.
What is a red flag for neck pain?
Red flags that require immediate medical evaluation include: neck pain after major trauma (like a car accident), fever or unexplained weight loss, severe unrelenting pain, progressive neurological deficits (numbness, weakness, especially in arms or legs), or loss of bowel/bladder control.
What are the red flags of hypertension?
Hypertensive red flags—symptoms of a potential crisis—include: severe headache, chest pain, severe anxiety, shortness of breath, nosebleeds, and significant changes in vision. If you have high blood pressure and experience these, seek urgent care.
What hurts when you have high blood pressure?
High blood pressure commonly causes a pressing headache, often at the back of the head. It can also cause chest pain (angina), muscle aches from reduced circulation, and generalised discomfort due to the strain on the cardiovascular system.
What three parts of the body can be damaged from high blood pressure?
The three primary organs damaged by untreated hypertension are the heart (leading to heart attack or failure), the brain (increasing risk of stroke and dementia), and the kidneys (causing chronic kidney disease or failure). The eyes and arteries are also major targets.
What are the silent signs of high blood pressure?
Often, there are none—hence the “silent killer” label. Subtle signs can include mild, persistent headaches, occasional dizziness, fleeting chest flutters, or more frequent nosebleeds than usual.
What does your head feel like when your blood pressure is high?
It often feels full, tight, or under pressure, especially at the back. Some describe a pulsating sensation or a dull, constant ache that is worse in the morning. For a deeper dive, read our article: What is a Hypertension Headache?
What are the four signs your heart is quietly failing?
Early signs of heart failure include: 1) Shortness of breath during activity or when lying down, 2) Persistent coughing or wheezing, 3) Swelling (oedema) in feet, ankles, legs, or abdomen, and 4) Unusual fatigue and weakness.
Why is hypertension the silent killer?
Hypertension is called the silent killer because it typically has no obvious symptoms for years while it silently damages blood vessels and organs (heart, brain, kidneys), dramatically increasing the risk of sudden, catastrophic events like stroke or heart attack.
How long can you live with untreated hypertension?
This varies greatly, but untreated hypertension can shorten life expectancy by 5-10 years or more. The damage is cumulative; the longer it is uncontrolled, the higher the risk of disabling or fatal complications.
What is the best time of day to check blood pressure?
The best times are in the morning, before taking medication and before eating or caffeine, and again in the evening. Take two readings 1-2 minutes apart while seated and rested. Consistency in timing is key for accurate tracking.
How does sleep position affect blood pressure?
Sleeping position can influence nocturnal blood pressure. Sleeping on your left side is often recommended as it may reduce pressure on key blood vessels and improve circulation. Poor sleep posture can also aggravate neck pain, indirectly affecting rest and stress levels.
Should I sleep if my blood pressure is high?
If you take a reading and it’s moderately high but you have no emergency symptoms (severe headache, chest pain, etc.), it is generally safe to rest or sleep. Stress and anxiety from worrying can elevate it further. If readings are consistently high upon waking, consult your GP.
What arm should you use for blood pressure?
Use the arm that consistently gives you a higher reading. Initially, measure both arms. If there’s a consistent difference of more than 10-15 mmHg, inform your doctor, and thereafter always use the arm with the higher reading for monitoring.
Why am I waking up after 5 hours of sleep?
Waking early can be linked to stress and anxiety, which are both triggers for high blood pressure. Furthermore, untreated sleep apnoea—a condition strongly linked to hypertension—can cause fragmented sleep and early waking. Discuss this pattern with your doctor.
Disclaimer:
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional, such as your GP or a consultant, for diagnosis and personalised treatment plans related to hypertension or any other medical condition. The information here is based on current UK guidelines and medical literature as of 2026.
