If you have high blood pressure, a new or severe headache can be frightening. Is it just stress, or a warning sign something is seriously wrong?
The term “hypertension headache” is used to describe a headache believed to be directly caused by very high blood pressure, often during a hypertensive crisis. Understanding this link is crucial for your health.
This guide, tailored for a UK audience, cuts through the confusion. We’ll explain what the science says, how to recognise the signs, and the clear NHS-recommended steps you should take.
Understanding the Link Between High Blood Pressure and Headaches

High blood pressure (hypertension) is often called the “silent killer” because it typically has no symptoms. According to Blood Pressure UK, most people with hypertension feel perfectly fine.
So, when do headaches come in? Medical experts, including the British Heart Foundation, note that headaches are not a common symptom of standard high blood pressure. They tend to occur only when blood pressure becomes severely and dangerously high—usually at a level that would constitute a hypertensive urgency or emergency.
In essence, a true “hypertension headache” is not a daily nuisance; it’s a potential red flag that your blood pressure has spiked to a critical level and requires immediate attention.
What Does a Hypertension Headache Feel Like? Recognising the Symptoms
User searches for “what do hypertension headaches feel like” or “hypertension headache back of head” point to a need for clear description. Symptoms can vary, but common reports include:
-
A pounding, pulsating sensation that beats in time with your heartbeat.
-
Pain that is often felt bilaterally (across both sides of the head).
-
A feeling of intense pressure or tightness, sometimes specifically at the back of the head and neck upon waking.
-
The headache is typically unresponsive to common over-the-counter painkillers like ibuprofen or paracetamol, or relief is very short-lived.
Crucially, this type of headache is usually accompanied by other signs of very high BP.
Concerned about your readings? Learn how to choose the best home blood pressure monitor in the UK for accurate tracking.
Key Warning Signs: When a Headache is a Medical Emergency
This addresses searches for “How to tell when a headache is serious?” and “Is hypertension headache dangerous?”.
A headache becomes a potential hypertensive emergency if it is sudden, severe, and accompanied by any of the following symptoms:
-
Blurred vision, double vision, or visual disturbances.
-
Confusion, disorientation, or difficulty speaking.
-
Chest pain or shortness of breath.
-
Nausea or vomiting.
-
Severe anxiety or a feeling of impending doom.
-
Nosebleeds.
NHS Urgent Advice: If you have a sudden, severe headache and any of these symptoms alongside a known history of high blood pressure, seek immediate medical help. Call 999 or go to A&E.
Common Triggers: What Causes a Hypertension Headache to Spike?

Understanding “what triggers a hypertension headache” helps with prevention. These headaches are often the result of blood pressure rising to extreme levels. Triggers can include:
-
Unmanaged or Untreated Hypertension: Simply not taking prescribed medication.
-
Acute Stress: A sudden, severe stressful event causing a massive adrenaline surge.
-
Certain Medications or Substances: Some decongestants, NSAIDs, caffeine, or illicit drugs.
-
Underlying Medical Conditions: Issues with the kidneys or adrenal glands.
-
Forgetting Medication: Non-adherence to your BP treatment plan.
Even common illnesses can affect your readings. Read our guide on whether a common cold can cause high blood pressure for more insight.
How to Get Rid of a Hypertension Headache: Safe Treatment Approaches

The search for “how to get rid of high blood pressure headache instantly” is dangerous if it leads to ignoring the cause. You cannot safely treat the headache without treating the high BP causing it.
-
Immediate Action: If you have symptoms of a hypertensive emergency (as above), call 999.
-
For a Severe Headache with High BP Reading: If you feel unwell, contact NHS 111 for urgent guidance. Do not try to “ride it out.”
-
Medication is Key: The only way to relieve a true hypertension headache is to lower the blood pressure safely. This is done under medical supervision, often with specific prescription medication. Do not take extra doses of your own medication without direct medical advice.
-
The Ibuprofen Question: Is ibuprofen good for hypertension headaches? No. Ibuprofen and similar NSAIDs can actually raise blood pressure and interfere with some BP medications. Paracetamol is a safer choice for general headache pain, but it will not treat the root cause.
Long-Term Management: Preventing Future Episodes
The best “treatment” is prevention through consistent blood pressure control.
-
Adhere to Medication: Take all prescribed medication as directed by your GP.
-
Monitor at Home: Use a validated upper-arm monitor. Use blood pressure average calculator Track your readings over time.
-
Lifestyle Modifications: Adopt a low-sodium diet, exercise regularly, maintain a healthy weight, and limit alcohol.
-
Manage Stress: Incorporate techniques like mindfulness or gentle yoga.
-
Prioritise Sleep: How does sleep affect blood pressure? Poor sleep, especially from sleep apnoea, can significantly elevate BP. Aim for 7-9 hours of quality sleep per night.
Feeling fatigued? Understand the link between hypertension and energy levels in our article, “Does High Blood Pressure Make You Tired?“
Understanding Your Diagnosis: What is Stage 1 Hypertension?
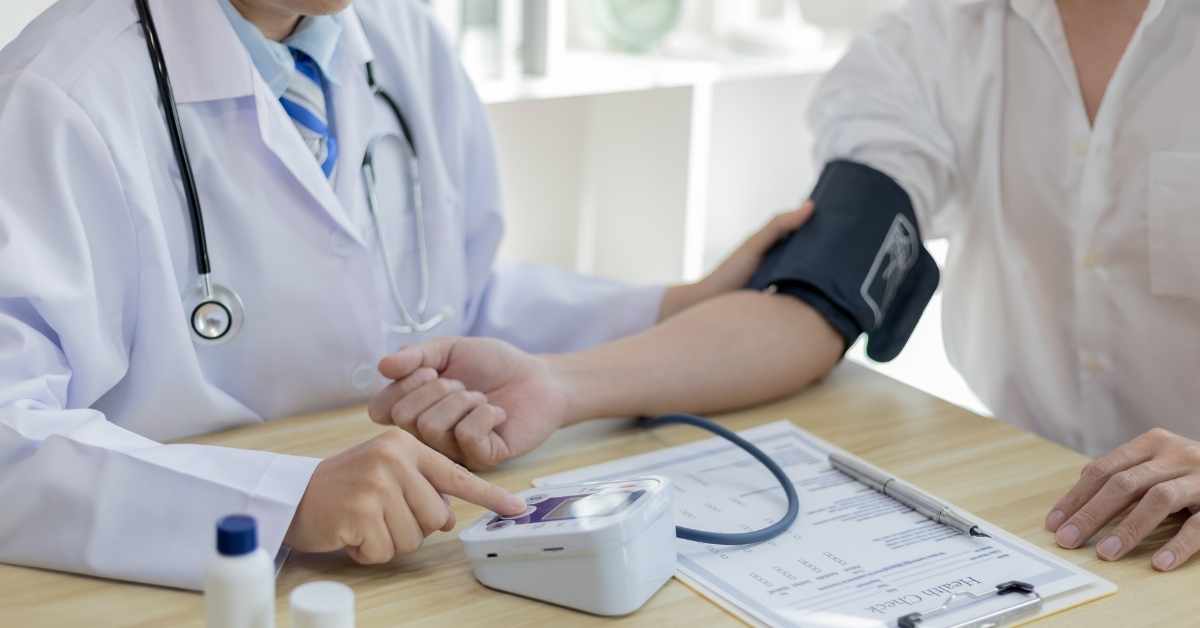
In the UK, hypertension is diagnosed in stages based on clinic and/or home readings.
-
Stage 1 Hypertension: Clinic readings of 140/90 mmHg or higher, or home readings averaging 135/85 mmHg or higher.
-
At this stage, lifestyle changes are paramount, and medication may be offered based on your overall cardiovascular risk.
A hypertension headache is extremely unlikely at Stage 1. It is associated with much higher readings, often exceeding 180/120 mmHg.
(Internal Link Suggestion: Place here) For accurate measurement, ensure you’re checking both arms. Learn about the reasons for differences in our piece, “Why Your Blood Pressure Can Be Different in Each Arm.”
FAQ
How do you get rid of a hypertension headache?
You must lower the dangerously high blood pressure causing it. This requires urgent medical assessment. Do not try to treat it at home with painkillers alone. Call 111 or, in an emergency, 999 for guidance and safe treatment.
What do hypertension headaches feel like?
They are often described as a severe, pounding, or pulsating pain, frequently felt across the entire head or at the back of the skull. The headache typically does not respond well to standard pain relief medication.
What are the symptoms of hypertension in the head?
Beyond the headache itself, symptoms can include dizziness, blurred or double vision, confusion, and ringing in the ears (tinnitus). These indicate very high pressure affecting the brain and require immediate medical attention.
What triggers a hypertension headache?
It’s triggered by a sudden, severe spike in blood pressure to dangerous levels. Common causes include missing hypertension medication, extreme acute stress, certain medications (like decongestants), or underlying health conditions affecting the kidneys or arteries.
How long do hypertension headaches last?
The headache will typically persist until the critically high blood pressure is lowered with appropriate medical treatment. It is not a headache that comes and goes quickly; it is a sustained symptom of an ongoing medical crisis.
What does your head feel like when your blood pressure is high?
With chronically high blood pressure, you usually feel nothing. During a dangerous spike (hypertensive crisis), you may feel a sudden, severe pounding headache, often with pressure at the back of the head, accompanied by visual changes, confusion, or nausea.
How to tell when a headache is serious?
Seek immediate help if a headache is sudden and explosive (“thunderclap“), is the worst you’ve ever had, is accompanied by fever, stiff neck, confusion, seizures, or weakness, or if it follows a head injury. With high BP, combine headache with chest pain, shortness of breath, or visual changes as red flags.
Is ibuprofen good for hypertension headaches?
No. Ibuprofen and similar anti-inflammatory drugs (NSAIDs) can raise blood pressure and reduce the effectiveness of some hypertension medications. Paracetamol is a safer choice for general pain but will not treat the underlying hypertensive crisis.
How will I feel if my BP is high?
Most of the time, you will feel normal, which is why regular checking is vital. Only during a severe hypertensive crisis might you feel a severe headache, chest pain, shortness of breath, anxiety, nosebleeds, or confusion.
What are the 10 warning signs of high blood pressure?
High blood pressure itself rarely has warning signs. However, signs of a hypertensive crisis include severe headache, nosebleeds, severe anxiety, shortness of breath, chest pain, irregular heartbeat, vision changes, blood in urine, pounding in chest/neck/ears, and confusion. Many of these require emergency care.
How does sleep affect blood pressure?
Blood pressure naturally dips during healthy sleep (nocturnal dipping). Poor sleep, especially from conditions like obstructive sleep apnoea, keeps your body in a stressed state, raising night-time and daytime BP. Consistently poor sleep is a significant risk factor for developing hypertension.
What is Stage 1 hypertension?
Stage 1 hypertension in the UK is diagnosed when your clinic blood pressure readings are consistently 140/90 mmHg or higher. It’s a clear signal to begin active intervention through lifestyle changes and, often, medication to prevent progression to more serious stages and reduce long-term cardiovascular risk.
